I think my husband and I are like that saying “I can’t keep my ducks in a row, I can’t even keep them in the same room!” That seems to be what’s been happening with us lately. Just as soon as I think we have something under control, something else goes out of whack. He’s been going to physical therapy twice a week for his back for several weeks now and it seems to be helping. What a relief that is, but because he is off on Mondays, he’s been making one of the weekly appointments for Monday. This week I figured that would be no big deal because his appointment was for early morning which would give us plenty of time to plan some kind of outing.

But my heart decided not to cooperate. As I was sitting in my recliner Saturday afternoon reading a book, I felt my heart beginning to race. Not a really big deal and not too alarming since I’ve been having small episodes like this for several weeks and it’s part of the heart’s healing process. In fact, I had had one episode the evening before, lasting only about 20 seconds or so. But this one did not go away. As soon as I realized my heart was beating fast, I started paying attention to the heartbeat in my ears (I’m lucky that way) and just by listening and doing my “one thousand one, one thousand two” counting, I knew that my heartbeat was well over 100 beats a minute. I got out my handy little Oxprovo handheld heart monitor (which I had relegated to the drawer after my last successful cardioversion because I was SURE it wasn’t going to happen again) and took a reading; 128 beats per minute. Damn. As the evening wore on, I got less and less hopeful that this episode would go away by itself and I was right, it didn’t. I waited all weekend, determined that this episode was not going to derail me or define my life and I was determined to act as if nothing was wrong. I went to my play practice Sunday night and even to exercise class on Monday morning. I was keenly aware of my heart rate during exercise class as my heart often went up to over 140 beats per minute which makes for some shortness of breath. I did what I could, and rested when I felt like a needed to. As soon as the class ended though, I called my doctor’s office and to my surprise, I received a return phone call within an hour, scheduling me to see the physician’s assistant the next day.
When I got to the appointment the next day and the nurse ran an EKG, which determined that my heart was again in Atrial Flutter (with 2:1 conduction) with a heart rate of 138 beats per minute.
Atrial Flutter is defined as: a common abnormal heart rhythm where the upper chambers (atria) of the heart beat too fast, which results in atrial muscle contractions that are faster than and out of sync with the lower chambers (ventricles).
After being examined by the PA, he said he needed to get my heart rate down and was going to again prescribe me a heart rate medication that I am sensitive to but at a low dose. Additionally, he wanted to change my heart rhythm medication to a medication I had previously taken last spring before my second cardioversion. I was dismayed at the thought of being told to take a low dose of medication that only at a high dose usually administered intravenously at the hospital was successful in converting my heart to a normal rhythm. I told him that I didn’t believe that such a small dosage of the heart rate medication would lower my heart rate. I told him I was pretty miserable and almost started to cry and asked him if we could do a cardioversion first and then worry about changing medications and to my surprise, he agreed. I was shocked when I was told they were going to schedule the cardioversion for the next day.
One of the hardest things to tolerate, along with the physical symptoms of Atrial Fibrillation and Atrial Flutter, is the constant uncertainty. When I am having an episode, in the back of my mind is always the fear that my heart rate will go past the point of where I can tolerate it; that I will dissolve into a panicked heap of crying mess, and I will have no choice but to go to the Emergency Department to have it dealt with there. Not that the Emergency Department is a bad place or anything, I just don’t want to go there. And then there’s what it does to my husband. Each time I’ve gone through something, he’s gone through it with me and powerless to do anything, he just has to sit and wait.
I got to the hospital at the assigned time only to find the outpatient waiting room completely filled. Not a good sign. We had to wait almost an hour past my appointed time. After getting in and getting prepped, we had to wait for my lab results to come back, and, since the results didn’t come back before the doctor began another procedure, we had to wait another hour. So all in all, we were running two hours late.
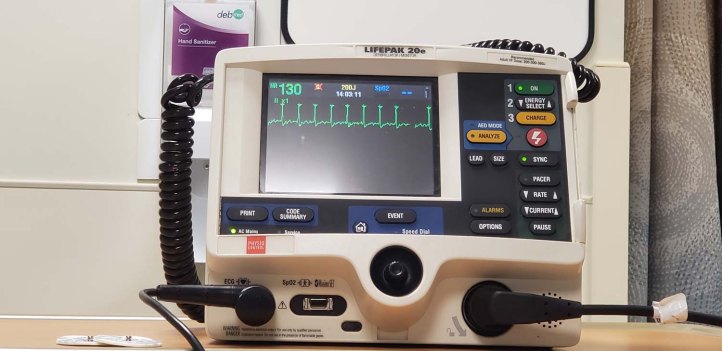
When I was first hooked up to the heart monitor, the nurse said she did not see atrial flutter; only a rapid heart rate. She then ran an ECG which also stated I was not in Atrial Flutter, but in Sinus Tachycardia.
Sinus Tachycardia is defined as: an elevated sinus rhythm characterized by an increase in the rate of electrical impulses arising from the sinoatrial node. … The normal resting heart rate is 60–100 bpm in an average male adult and 60-90 bpm in an average female adult.
In other words, it’s a fast but normal rhythm. My heart (which was beating rapidly) fell. Does this mean they wouldn’t do the cardioversion and I’ll have to continue to endure this rapid heart rate? She said she would have to check with the Electrophysiologist to make a final determination since the two arrhythmias look very similar on an ECG reading. She came back a few minutes later and said the doctor determined it was Atrial Flutter. I never thought I’d be relieved to hear that, but it meant that definitely, I would get the cardioversion and an almost assurance that my heart rate would be returned to normal.
The reason for this misinterpretation according to https://www.ems1.com, Atrial Flutter with 2:1 conduction is one of the most, if not the most, misdiagnosed dysrhythmias in all settings. When atrial flutter is conducted 2:1, the resulting ventricular rate (ventricles are the lower chambers of the heart) is around 125-175 per minute (which is the number you see on the monitor) . This is because the P waves (flutter waves) in atrial flutter occur at about 250-350 per minute (usually around 300 which is why it is called 2:1, atrial rate is two times the ventricular rate).
At this rate, it can appear that there is a P wave in front of each QRS and a T wave after each QRS. This causes the misdiagnosis of sinus tachycardia.
The interpretive algorithms of ECG machines often get atrial flutter with 2:1 conduction wrong, just like people do.
Additionally, most people with sinus tachycardia, especially over 130 bpm, will usually have a readily-apparent reason for the tachycardia, like fever, fear, pain, anxiety, exertion, drugs, hypovolemia or hypoxia.
Finally, the results were in, the doctor was ready and two and a half hours late, the procedure began. The cardioversion is always done under propofol sedation. That’s such a handy little drug. It’s such an odd sensation to feel wide awake one minute and then in about 15 seconds begin to feel as though you were sinking into a fluffy cloud, then poof, nothing until you wake up. This time the procedure took a little more than the usual ten minutes because my heart wasn’t cooperating with the doctor either. He said later that after he had given my heart the shock, my heart continued to flip in and out of flutter, finally settling down into a normal rhythm. But still, it was only 20 minutes. An hour later we walked (or I should say, my husband walked and I got to ride in the metal chariot) out the door and on to dinner. (And we were starved, my breakfast was at 4:30 a.m. and his was just a little later).

My fingers are crossed for next week that we can do something fun, that his back will continue to feel better and my heart decides to play nice.
